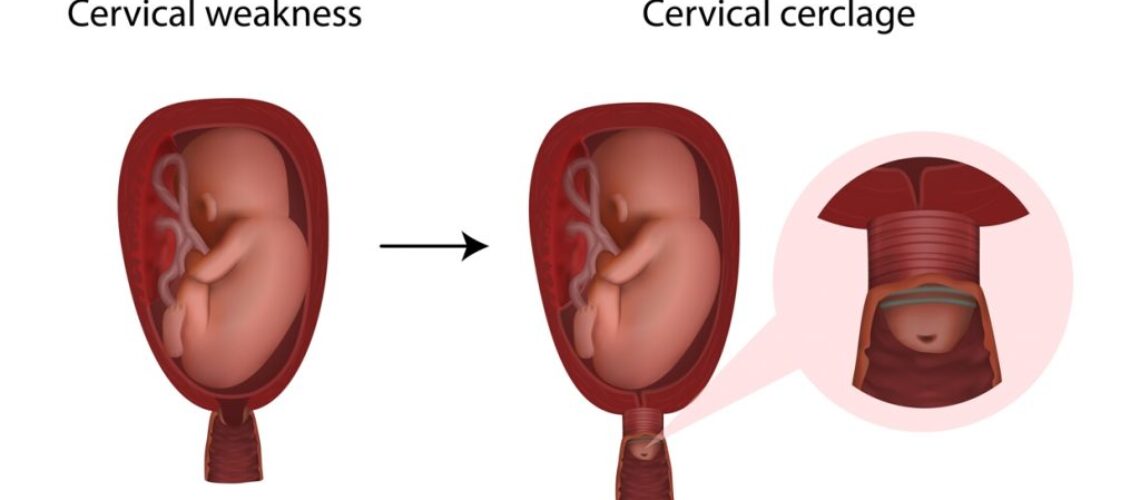
What is a cervical cerclage?
A cervical cerclage is an operation where a stitch is placed around the cervix (neck of the womb). It can be done between 12 and 24 weeks of pregnancy.
Who might need a cervical cerclage?
- Women who have delivered a baby before 34 weeks of pregnancy.
- Women who have 1 or more miscarriage after 14 weeks of pregnancy.
- Women who have a short cervix on ultrasound. This means an internal scan has shown your cervix is <25mm or has been shortening significantly since the start of your pregnancy.
- Women who have had cervical procedures such as 2 LLETZ procedures or a cone biopsy.
The purpose of the stitch is to reduce the risk of your baby being born early. A cervical stitch helps to keep the cervix long and closed, thereby reducing the risk of preterm birth or late miscarriage.
How will the cervical stitch be put in?
The stitch is inserted in an operating theatre. This is done under spinal anaesthetic where you will stay awake but will be numb from the waist down.
You will need to fast from midnight the night before the procedure. You should come in to the admissions office at 7.30am the morning of the procedure. If you are taking regular medications you should discuss this with the doctor. Most medications can be taken with a sip of water on the day of the procedure.
In the operating theatre, your legs will be put in supports and sterile covers will be used to keep the operating area clean. The doctor will then insert a speculum (a metal instrument used to separate the walls of the vagina and see the cervix) into the vagina and put the stitch around the cervix. The operation should take less than 30 minutes.
After the procedure you will have a catheter (tube in the bladder) for a few hours until the spinal anaesthetic wears off and you have normal sensation. You may need to stay overnight. However, some women go home the same day as the procedure. You will have an ultrasound examination to check your baby’s heartbeat after the procedure.
What might I expect afterwards?
After the operation, you will usually have some bleeding from the vagina, which should change to brown in colour after a day or two. Some women also experience crampy abdominal pain.
Once you recover from the operation, you can carry on as normal for the rest of your pregnancy. Resting in bed is not normally recommended. Your doctor can advise you about the activities you can do and those best avoided.
Is there anything I should look out for?
If you experience any of the following symptoms, you should contact the hospital:
- contractions
- heavy vaginal bleeding
- your waters breaking
How and when will the stitch be taken out?
Your stitch will be taken out at the hospital. This will normally happen at around 36–37 weeks of pregnancy.
You will not normally need an anaesthetic. A speculum is inserted into your vagina and the suture is cut and removed. It usually takes just a few minutes.
You may have a small amount of bleeding afterwards. Any red bleeding should settle within 24 hours but you may have a brown discharge for longer.
If you go into labour with the cervical stitch in place, it is very important to have it removed promptly to prevent damage to your cervix. If you think you are in labour you should attend the hospital.
If your waters break early but you are not in labour, the stitch will usually be removed because of the increased risk of infection.